Spinal Stenosis Treatment in Bergen County, NJ
Spinal stenosis narrows the spinal canal — the bony tunnel that protects your spinal cord and nerve roots. When that tunnel gets tight, the nerves inside get squeezed. That pinching causes the pain, numbness, weakness, or “heavy legs” feeling that brings most patients through our doors. The good news: the majority of spinal stenosis cases respond to conservative, non-surgical care — especially when treatment starts before symptoms become severe.
What is spinal stenosis?
Your spine isn’t just a stack of bones — it’s a protective tunnel running from the base of your skull to your tailbone, with the spinal cord and nerve roots threading through it. Specifically, spinal stenosis happens when the inside of that tunnel narrows, leaving less room for the nerves. The narrowing can come from bone spurs, thickened ligaments, herniated disc material, or simply decades of degenerative wear.
There are two main types of spinal stenosis based on where the narrowing happens:
Lumbar spinal stenosis
Affects the lower back. Squeezed nerves typically refer symptoms into the buttocks, thighs, and legs. Many patients first notice it when walking or standing for more than a few minutes — the legs start aching, going numb, or feeling weak, and sitting down brings relief. This pattern has a name: “neurogenic claudication.”
Closer monitoring
Cervical spinal stenosis
Symptoms of spinal stenosis
Spinal stenosis is a slow-burn condition. In fact, most people develop it gradually over years, and it often starts as something easy to dismiss — a little tightness after a long walk, a leg that “falls asleep” too easily. Pay attention to symptoms that follow these patterns:
- Leg pain, cramping, or heaviness when walking or standing — that gets noticeably better when you sit down or lean forward (e.g., on a shopping cart)
- Numbness or tingling in the buttocks, thighs, or feet
- Weakness in the legs — feeling like your legs are “giving out” or having to grab a rail to climb stairs
- Lower back pain that may or may not be the dominant symptom
- Walking distance decreasing — finding yourself measuring routes by where you can sit and rest
- Numbness, tingling, or weakness in the arms or hands — sometimes one-sided, sometimes both
- Difficulty with fine motor skills — buttoning shirts, writing, handling small objects
- Balance and coordination changes — tripping more often, feeling unsteady
- Neck pain that may radiate into the shoulders or upper back
- In advanced cases: changes in bowel or bladder function (rare but warrants immediate medical attention)
Don’t wait — see a doctor right away if you have:
Most spinal stenosis develops slowly enough that there’s time to pursue conservative care. But certain symptoms need a medical evaluation right away — not to scare you, just to be safe:
- Sudden, severe weakness in the legs or arms
- Loss of bowel or bladder control
- Numbness in the groin or “saddle” area
- Rapidly progressing symptoms over days rather than months
If any of those apply, see a doctor or go to an ER before booking conservative care.
What causes spinal stenosis?
Osteoarthritis & bone spurs
As cartilage in the spinal joints wears down, the body grows bone spurs that take up space in the canal
Previous injury or surgery
Old trauma or scar tissue
Spondylolisthesis
When one vertebra slips forward over another, narrowing the canal
Congenital narrow canal
Some people are born with a narrower-than-average spinal canal, which means stenosis can develop earlier
Herniated or bulging discs
Disc material pushed into the canal narrows the available space
Less common
Tumors, infections, Paget's disease, or other systemic conditions
Thickened ligaments
The ligamentum flavum, which runs along the back of the spinal canal, can thicken with age and bulge inward
How We Identify Your Cause
Non-surgical spinal stenosis treatment at Spine & Health Center
For most patients with mild-to-moderate spinal stenosis, conservative non-surgical care is the first-line approach — and often the only treatment that’s needed. We reserve surgery for severe or progressive cases only. As a result, our clinics combine multiple non-surgical modalities so we can address the underlying mechanics, not just the symptoms.
1. Spinal decompression therapy
Mechanical spinal decompression therapy uses precisely controlled traction to gently stretch the spine, creating negative pressure that can pull bulging or herniated disc material away from compressed nerves. For lumbar stenosis with disc involvement, decompression therapy often delivers meaningful symptom relief over a course of sessions. We use protocols matched to your specific findings — not a one-size-fits-all package.
2. Physical therapy and targeted exercise
3. Chiropractic care
4. Class IV laser therapy
Posture, movement, and lifestyle
When surgery may be necessary
We are a non-surgical clinic, but we won’t pretend surgery is never the right call. For a small number of patients — usually those with severe progressive weakness, persistent bowel or bladder dysfunction, or unrelenting neurological symptoms despite full conservative care — surgical decompression (laminectomy or fusion) is the appropriate next step.
If your case warrants it, we’ll tell you. We work alongside surgeons in the area for the small subset of cases that need them. For most patients, that’s a conversation we never have to have.
Where non-surgical care has limits
Non-surgical care works well for most stenosis patients, but it has limits we want you to know about up front. Conservative care typically does NOT resolve:
- Severe, progressive motor weakness (foot drop, hand weakness, grip loss)
- Bowel or bladder dysfunction associated with leg or arm symptoms (a possible cauda equina sign this needs urgent ER evaluation, not chiropractic care)
- Loss of sensation in the saddle/genital region
- Worsening neurological deficits despite 4-6 weeks of focused conservative care
In any of those situations, we recommend neurosurgical consultation immediately. We can coordinate the referral.
For everyone else the much larger group with classic neurogenic claudication (leg pain worse with walking, relieved by sitting or leaning forward) or cervical radiculopathy without severe motor loss conservative care is the right first step and often the only step needed. Studies consistently show that non-surgical care is comparable to surgery for moderate stenosis at 2-year follow-up, with significantly lower risk and faster return to activity. The decision point is whether symptoms are progressing, not whether they exist.
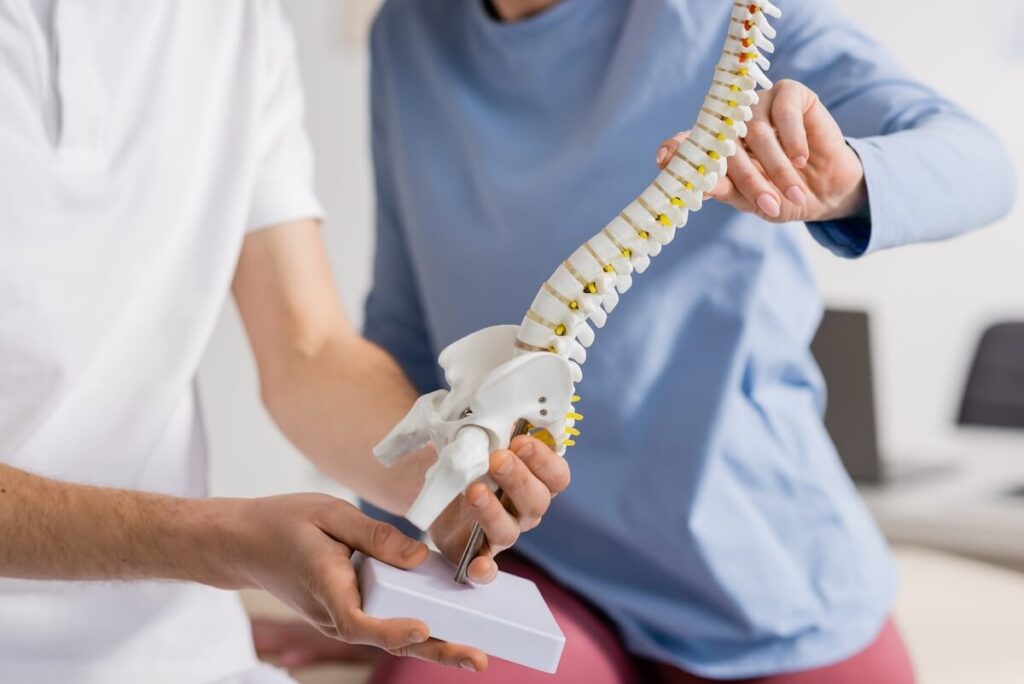
What to expect at your first visit
-
A full history — when symptoms started, what makes them better or worse, what you've tried, what's working and what isn't
-
A physical exam — testing strength, reflexes, sensation, range of motion, and walking pattern
-
A review of any imaging you've already had (MRI, X-ray, CT) — bring it on a disc, USB, or patient portal access
-
A treatment plan tailored to your severity and goals
If you haven’t had imaging and your provider thinks it’s needed, we’ll refer for an MRI before starting active treatment. For mild or early-stage stenosis, conservative care can often start the same day.
Most patients begin with 2 to 3 visits per week for the first few weeks, tapering as symptoms improve. We re-evaluate progress every few weeks and adjust the plan based on what’s working.
Why Choose The Spine and Health Center for Spinal Stenosis
Spinal stenosis is one of the most undertreated chronic spine conditions in Bergen County patients often bounce between primary care, pain management, and orthopedic consultations for months or years before finding a coordinated non-surgical plan. Three things shape how we work with stenosis patients:
First, we treat stenosis with a layered non-surgical plan, not a single modality. Spinal decompression therapy, targeted physical therapy, chiropractic care, and Class IV laser therapy each address a different driver of stenosis-related pain and most patients need a combination, not just one. We sequence the layers by what your symptoms and imaging actually call for, not by what we have available.
Second, we honestly screen for whether non-surgical care is the right path. Stenosis isn’t always a candidate for conservative care. Patients with progressive neurological deficits, severe motor weakness, or red-flag symptoms (bowel/bladder changes, saddle anesthesia) need urgent neurosurgical evaluation not chiropractic care. We say so on the first visit, and we coordinate the referral when it’s the right call.
Third, we re-evaluate every 4-6 sessions and tell you honestly whether the plan is working. If conservative care isn’t reducing your symptoms measured by walking distance, leg/arm symptoms, and functional capacity we adjust the plan or refer out. We don’t run open-ended care plans for stenosis.
Our licensed chiropractors and Doctors of Physical Therapy each have documented training in non-surgical spine care delivered across our three Bergen County offices in Closter, Montvale, and Park Ridge with patients regularly traveling from Haworth, Emerson, Bergenfield, Westwood, River Edge, Hillsdale, Harrington Park, Glen Ridge, and Essex Fells.
Same week appointment availability is typical.